Despite the fact that vitamin D, frequently referred to as the “sunshine vitamin,” is essential for good health, billions of people worldwide lack it. The lack of this vital vitamin has become a quiet epidemic as eating patterns shift and indoor living becomes more common. The complexities of vitamin D deficiency are examined in this article, along with its causes, signs, dangers, and workable preventative and therapy plans. By bringing attention to this problem, we hope that readers will be able to identify and take care of this widespread yet usually disregarded health condition referred to as Deficiency.
What is vitamin D and why is it important?
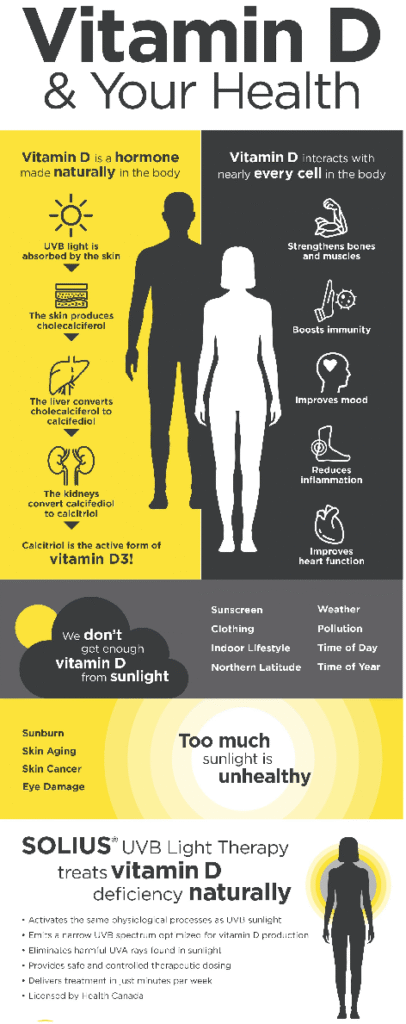
When ultraviolet B (UVB) rays from sunshine contact our skin, our bodies naturally manufacture vitamin D, making it unique among vitamins. There are two main types of it: vitamin D2 (ergocalciferol), which is found in some plants and fungi, and vitamin D3 (cholecalciferol), which is produced in the skin or obtained from animals. Once activated in the liver and kidneys, it changes into calcitriol, a hormone that regulates calcium and phosphorus intake and is vital for bone health. Addressing vitamin D Deficiency is crucial for maintaining overall health and preventing related diseases.
In addition to bones, vitamin D affects mood, muscle function, and immune system function. It enhances cardiovascular health, reduces inflammation, and lowers the risk of several types of cancer. These systems are upset by deficits, which results in a variety of health issues. Medical professionals say that preventing chronic illnesses requires maintaining appropriate levels, which are normally 20–50 ng/mL in blood tests.
Vitamin D Deficiency Causes:
Low vitamin D levels are caused by a variety of reasons, many of which are related to contemporary living. Primarily, people who live in northern latitudes, work in offices, or cover their skin for cultural or protective reasons do not get enough UVB rays. Although sunscreen is necessary to prevent skin cancer, excessive use of it inhibits the synthesis of vitamin D.
An further factor is inadequate nutrition. There are several meals that don’t naturally contain vitamin D, and not everyone eats fortified foods like milk or cereal. Since fatty fish and egg yolks are the main sources of vitamin D3, vegetarians and vegans may have difficulties. Nutrient absorption is hampered by malabsorption problems, such as those that occur in celiac disease or following gastric bypass surgery. Anticonvulsants and glucocorticoids are two examples of drugs that hasten the degradation of vitamin D. It is less efficiently produced by the epidermis in older adults, and its conversion to its active form is more challenging due to declining renal function.
Because vitamin D is fat-soluble and stored in adipose tissue, obesity makes the situation worse by lowering its bioavailability. Because melanin acts as a natural sunscreen, darker skin tones need more exposure to the sun. Finally, chronic diseases such as renal or liver disease directly affect metabolism.
The Silent Warning Symptoms and Signs:
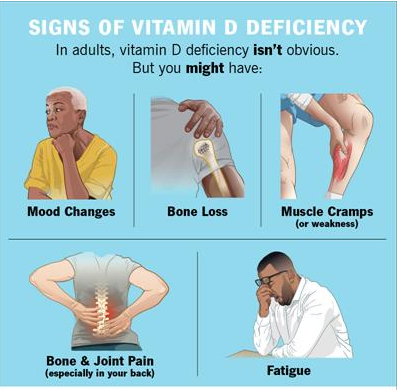
Vitamin D deficiency can occasionally go undetected because of symptoms that resemble those of other illnesses. Adults with chronic fatigue may find routine tasks to be draining. Muscle weakness and cramping may result in difficulty ascending stairs or frequent falls. Osteomalacia, a disorder in which bones deteriorate as a result of inadequate mineralization, is indicated by bone pain, especially in the lower back, hips, or legs.
Low levels of vitamin D have been connected to mood swings including anxiety and depression because it is involved in the production of serotonin. Recurrent infections, poor wound healing, and hair loss are signs of weakened immunity. A significant deficit causes rickets, which shows up in youngsters as bowed legs, delayed growth, and skeletal deformities.
Because these symptoms are typically not evident, blood testing are advised for at-risk individuals, including the elderly, expectant mothers, and people with limited sun exposure.
Health Hazards: Not Just Bones:
If treatment is not received, the deficit deteriorates into major problems. The risk of fractures is increased by osteoporosis, particularly in postmenopausal women. Because vitamin D lowers inflammation and helps regulate blood pressure, cardiovascular problems including heart disease and hypertension are becoming more common.
Low levels have been linked to an increased risk of diabetes through impaired insulin sensitivity and may worsen inflammatory conditions like rheumatoid arthritis or multiple sclerosis. Studies indicate a link between seasonal affective disorder and mental health conditions. In severe circumstances, it may contribute to chronic pain syndromes or possibly some types of cancer, though more research is required.
Global Prevalence: An International Issue
Over a billion people worldwide suffer from vitamin D insufficiency, making it a global problem rather than a local one. The Middle East, where exposure is limited by traditional attire, and northern Europe, where winters are long, are high-risk regions. Lack of skin pigmentation affects more than 40% of Americans, with a prevalence of over 70% among African Americans and Hispanics.
Urbanization and pollution exacerbate the issue in emerging nations. Global comparisons show glaring differences, with rules governing food fortification causing significant variations in nutritional supplies.
Prevention: Diet and Sunlight:
The first line of defense against deficiency is balanced sun exposure, which should be 10 to 30 minutes at midday, several times a week, depending on skin type and location. Steer clear of extended exposure to prevent skin damage.
Incorporate vitamin D-rich foods: Fatty fish, including salmon or mackerel, contain 400–600 IU per serving, and readily accessible sources include cereals, orange juice, and fortified dairy. For vegans, UV-treated mushrooms and egg yolks are OK. For those who are at risk, supplements are recommended, usually 600–2000 IU daily; nevertheless, see a doctor to avoid toxicity. Lifestyle changes like using UV lights or going for a winter walk outside can help maintain levels.

The remedy is to get the body’s balance back:
As part of the treatment, supplements are administered under a physician’s supervision. While severe deficiencies may require high-dose therapy (50,000 IU per week) for 8–12 weeks, followed by maintenance, mild instances can be handled with 1000–2000 IU per day. To ensure efficacy, blood levels are tracked.
Addressing the underlying causes, such as dietary modifications or malabsorption, is essential. Children with rickets can avoid permanent problems if they receive therapy early.
Finally, a call to action:
Despite being common, vitamin D insufficiency is mostly preventable and treated. We can lessen its effects by encouraging nutrient-dense diets, sun-smart behaviors, and routine exams. The importance of this vitamin is highlighted by the growing understanding of its wider impacts, which range from immune system function to mental health. For a better future, embrace the sunshine vitamin and don’t let it fade.
Wow, fantastic blog layout! How long have you been blogging for? you made blogging look easy. The overall look of your web site is magnificent, let alone the content!
This is such an informative and much-needed awareness article! Many people underestimate how essential Vitamin D is—not just for bone health but also for immunity, heart function, and mood regulation. I like how this article clearly explains both the causes and preventive steps, combining science with practical lifestyle advice. It is a great reminder that small daily habits—like safe sunlight exposure and balanced nutrition—can make a huge difference to our long-term well-being.
I see something really interesting about your weblog so I saved to my bookmarks.